For thousands of years, humans have looked at the terrifying complexity of the body and asked, “How do I fix this?” In our quest for answers, we have built two great distinct streams of thought. One is built on ancient tradition, intuition, and the accumulated knowledge of ancestors. The other is built on a radical, often uncomfortable idea: we might be wrong, so let’s test it.
In this article, without being arrogant, we try to understand both the sides of the story, and ultimatley the story of the transition from Traditional Medicine (like Ayurveda) to Evidence-Based Medicine (EBM). This should not be labeled as a “West vs. East” in any way. It is a story of “Method vs. Assumption.”
Let’s try to analyze this by answering some of the popular questions associated with both the methods.
What is Modern Evidence-Based Science?
To understand modern medicine, we must understand that ‘Science’ or ‘Scientific Thinking’ is not just a body of knowledge. It is an endless series of making mistakes – correcting – making mistakes and correcting and so on. As Richard Feynman famously said, “Science is the belief in the ignorance of experts.” So the very fundamentals hypothesis of Science is that experts might be wrong.
Evidence-Based Medicine (EBM) is the careful, explicit, and judicious use of current best evidence in making decisions about the care of individual patients. It is a relatively young concept in its formal definition, but its roots lie in the rejection of authority.
The Figures from the Timeline of EBM
- The Ancient Roots: Hippocrates (400 BCE) tried to separate medicine from religion, arguing that epilepsy was physical, not divine. As a symbol of his legacy, often doctors today take the Hippocratic Oath to begin their journey in the medical sciences.
- The Ignaz Semmelweis Moment (1847): In the long history of EBM, if we are going to name three names, one should be Ignaz Semmelweis. He realized a simple thing we do (I hope you do too) – washing hands reduces infections. This is especially true while delivering a baby – lowering the post-birth infection among new mothers. He saved tons of mothers from childbed fever. In 1847, he proposed hand washing with chlorinated lime solutions at Vienna General Hospital’s First Obstetrical Clinic, where doctors’ wards had thrice the mortality of midwives’ wards. The maternal mortality rate dropped from 18% to less than 2%. This might not sound a significant achievement but at that time this was a revolutionary idea. He had data, but he lacked a mechanism (germ theory), so he was mocked. This was the dark age before EBM took hold.
- The Statistical Revolution (1940s-50s): If we are talking about the difference between traditional methodology and EBM, we have to understand Randomized Controlled Trial or RCT. Sir Austin Bradford Hill formalized the RCT.
In the vast, teeming jungle of medical claims, distinguishing a true cure from mere coincidence is a formidable challenge. To navigate this, science has evolved a rigorous tool, the Randomized Controlled Trial.
Imagine a group of patients, all seeking relief. We divide them, not by choice or preference, but by the impartial toss of a coin. One group receives the new treatment, the other, a placebo, a mimic (may be just a no-effect candy which looks like a medicine), indistinguishable from the real thing.
We then watch. And wait.
By removing human bias, any difference we observe in their recovery reveals the treatment’s true nature. It is the gold standard of evidence. A beacon of clarity that allows us to separate fact from folklore, ensuring that when we intervene in the delicate balance of the human body, we do so not with hope alone, but with certainty. We eliminate the most dangerous variable in the universe: human bias. We bring in rationality.
Three Post-1950 Success Stories of EBM
If you are reading this and you are over 40, you likely owe your life, or at least your quality of life, to these victories.
1. The Eradication of Smallpox (1980) This is arguably one of the greatest achievements of the human species, surpassing the moon landing. Smallpox killed 300 million people in the 20th century alone. There was existing traditional medicine which failed and chanting to different Gods in different countries did not serve as well. It was cured by a global, rigorously organized vaccination campaign based on immunology. In 1967, the WHO began an intensified eradication program. By 1980, the disease was gone.
- The Evidence: Zero natural cases of Smallpox have occurred since.
2. The Taming of HIV (1996 – Present) In the 1980s, HIV was a death sentence. There was panic, stigma, and snake oil (magical fraud solutions). But in the labs, scientists broke the virus down to its molecular components. By the mid-90s, Antiretroviral Therapy (ART) was introduced.
- The Result: A 20-year-old diagnosed with HIV today, with proper adherence to ART, has a life expectancy close to that of the general population. We turned a plague into a manageable chronic condition through molecular biology and clinical trials.
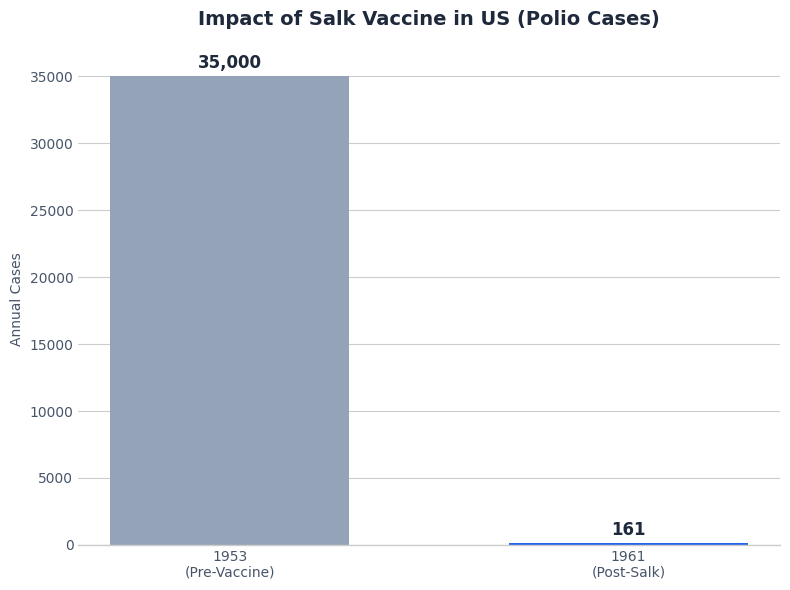
3. The Salk Polio Vaccine (1955): In the mid-twentieth century was terrifying a large global population.
Enter Jonas Salk, a researcher working not in the wild, but in the quiet confines of a Pittsburgh laboratory. Many scientists were hunting for a vaccine using a weakened, living virus but Salk took a different, controversial path. He believed he could teach the human immune system to defend itself using a killed virus, a mere ghost of the predator.
He tested this concoction on himself, his wife, and his own children. But to prove it to the world, a massive migration of data was needed. If it were traditional medicine, he would have stopped there and started minting money.
Over 1.8 million children participated. The data was processed not by intuition, but by punch cards and statistical analysis.
When the results were finally announced, declaring the vaccine “safe, potent, and effective”. A human plague had been tamed. And when asked who owned the patent to this life-saving discovery, Salk displayed a rare species of altruism. He simply replied, “There is no patent. Could you patent the sun?”
- The Result: Polio cases in the US dropped from 35,000 in 1953 to 161 in 1961. We are currently on the verge of eradicating it globally.
2. What is Traditional Medicine?
Before we had microscopes, we had observations. Traditional Medicine (TM), whether Ayurveda in India, Traditional Chinese Medicine (TCM), or the healing arts of ancient Egypt was humanity’s first attempt to hack the biological code. It was a genuine attempt by bright minds, but a primitive one.
Ayurveda, dating back over 3,000 years. Dr. Paphulla Chandra Ray, an eminent Chemist and researcher of ancient Chemistry writes in his book ‘A History of Hindu Chemistry’ that
We now alight upon a period when we find the Hindu system of Medicine methodised and arranged on a rational basis with scientific terminology. The two great works of this period are the Charaka and the Sususruta. In them we find the study of the subject to have made a distinct advance and to have been evolved out of the chaotic state it was in during the Vedic period. Of the two, the Charaka is by far the more ancient.
Dr. P. C. Ray, Chapter II of A History of Hindu Chemistry
There must have been a wide gap between the age of the A.V. (Atharva Veda) and that of the Charaka – an interval of probably a thousand years or more. In the latter the humoral pathology is fully developed, the diagnosis and prognosis of the diseases described at length, and an elaborate mode of classification adopted. We have seen above that the physicians were assigned rather an inferior status in society; the healing art was, in fact, never recognised as a division of the Vedas. Still the claims of the indispensable science of medicine which can be distinctly traced to A.V., could not altogether be ignored, and ultimately a compromise was arrived at. In the Charaka itself the Science of Life (Ayurveda) is regarded as a secondary or subsidiary branch (upanga) of the Atharvan and as a direct revelation of the gods. (Sutra Ch. XXX. 8-9)
The Susuruta even goes a step further and asserts that the self-existent (Brahma) created Ayurveda, as an Upanga of the Atharvan.
So Ayurveda started with a mixture of rational scientific methodology and divine interruption. Nevertheless, it was a bold effort.
Ayurveda posits that health is a balance of three Doshas (Vata, Pitta, Kapha). It was, for its time, revolutionary. The Sushruta Samhita contains descriptions of surgical procedures, including rhinoplasty (reconstructing the nose), which were centuries ahead of their time.
Egyptian Medicine (recorded in the Ebers Papyrus, c. 1550 BCE) used moldy bread to treat infections, thousands of years before Fleming discovered Penicillin. They didn’t know why it worked (fungi killing bacteria), but they observed that it somehow worked.
Three Post-1950 Success Stories of Traditional Medicine
It is arrogant to claim traditional knowledge is useless. When traditional knowledge is subjected to the rigorous testing of EBM and goes through proper Random Control Trial, we sometimes find gold.
1. Artemisinin (The Nobel Prize Winner) Tu Youyou, a Chinese scientist, turned to ancient TCM texts to find a cure for Malaria. She found a reference in a 4th-century handbook regarding Artemisia annua (Sweet Wormwood). The key was the extraction method (cold water, not boiling).
- The Success: Artemisinin became the standard treatment for malaria, saving millions of lives. Tu Youyou won the Nobel Prize in 2015. Note: She didn’t use the raw herb; she isolated the active molecule and proved it worked via science.
2. Arsenic Trioxide for Leukemia In Traditional Chinese Medicine, arsenic was a known poison also used for various ailments. In the 1970s, Chinese researchers discovered its specific efficacy in treating Acute Promyelocytic Leukemia (APL).
- The Success: Today, Arsenic Trioxide is an FDA-approved, frontline chemotherapeutic agent for APL, turning a once-fatal cancer into a highly curable one.
3. Reserpine from Rauwolfia serpentina In India, particularly in Ayurveda, the Sarpagandha plant was used for centuries for insanity and snakebites. In the mid-20th century, scientists isolated Reserpine.
- The Success: It became the first major drug to treat high blood pressure and psychosis. While largely replaced by newer drugs with fewer side effects, it was the “mother” of modern anti-hypertensives.
3. If Traditional Medicine is So Good Why Did We Move On?
If Ayurveda and Traditional Chinese Medicine were so great, why did we switch to Evidence Based Medicine?
We didn’t switch because we hated tradition. We switched because we started counting.
The Limitation of Anecdote: In the old days, if your village healer gave you a root and you got better, that was proof. But the human body has an amazing immune system. Most people get better on their own. Traditional systems took credit for the body’s natural recovery.
The Mechanism Gap: Ayurveda works on the theory of Doshas. But when we cut open a body, we can find veins, nerves, and lymph nodes. We cannot find a “Vata.” Germ theory provided a mechanism that explained why things happened. You couldn’t balance a “Kapha” imbalance to cure Cholera, but you could kill the Vibrio cholerae bacteria.
The Standardization Problem: One Vaidya’s (healer’s) powder is different from another’s. Evidence Based Medicine demands that 500mg of Paracetamol is exactly 500mg, whether you buy it in Mumbai, New York, or Tokyo.
We moved to EBM because it works faster, more consistently, and for more severe conditions. You can treat a mild cough with ginger tea (Ayurveda). You cannot treat a burst appendix or a myocardial infarction or brain stroke with ginger tea or any such Ayurvedic remedies.
4. What’s Wrong with Modern Medicine (and Pharma)?
Despite EBM’s contribution towards a better humankind, it has flaws. EBM is performed by humans, and humans are greedy, biased, and flawed. Ben Goldacre’s seminal book Bad Science exposes the rot in the floorboards.
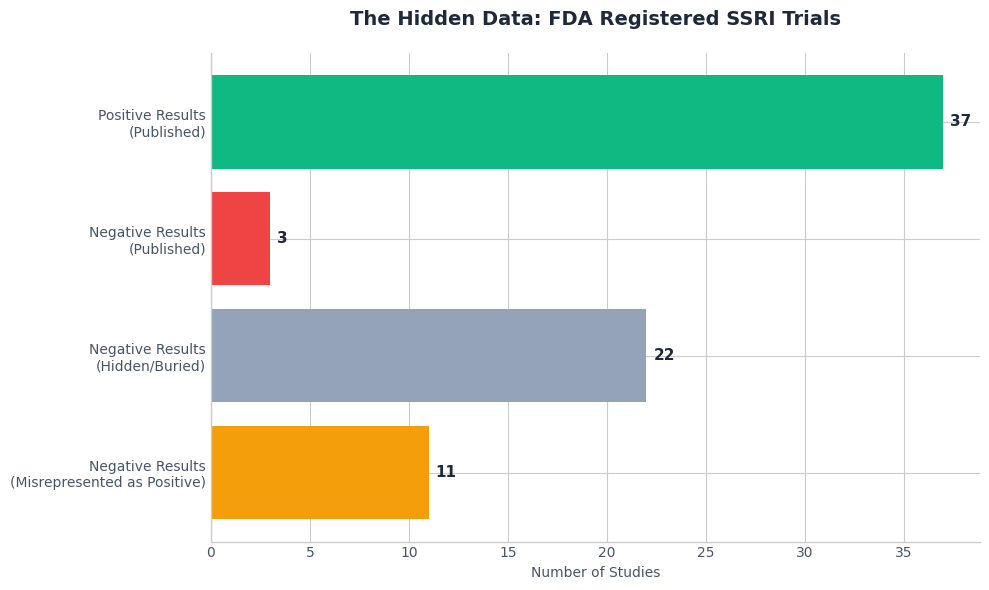
1. The “File Drawer” Problem (Publication Bias) Pharmaceutical companies fund trials. If the drug works, they publish it. If it fails, they often hide the data in a “file drawer.”
- The Data: A study on antidepressants (SSRIs) showed that out of 74 FDA-registered studies, 37 out of 38 positive studies were published. But of the 36 negative studies, 22 were not published, and 11 were written up to look positive. (Source: New England Journal of Medicine, Turner et al., 2008).
2. P-Hacking and Statistical Fraud: Researchers sometimes manipulate data to get a “p-value” below 0.05, the magic number for statistical significance. They measure 20 different outcomes and keep the one that looks like a “hit” by pure chance.
It is easier to understand what p-value actually is. In the high-stakes ecosystem of medicine, distinguishing a true life-saving signal from the background noise of chance is critical. To do this, scientists track a subtle mathematical footprint, the p-value.
[We begin by assuming a new treatment does nothing, a state known as the ‘Null Hypothesis.’ The p-value calculates the likelihood that the results we observe could have occurred by sheer accident. If this number is high, we must concede that our results are likely a fluke – it actually does nothing. But if it falls below a critical threshold, traditionally, five percent, or 0.05, we witness something significant. It suggests that the results are so rare, so unlikely to be random, that a real force must be at work.
For the medical community, this tiny decimal is a stern gatekeeper. It ensures that before a treatment reaches a human patient, we have rigorously ruled out the role of luck, placing our trust instead in the solid ground of evidence.]
3. The Vioxx Scandal This is the darkest hour of modern pharma. Merck marketed Vioxx for pain. Their internal data showed cardiovascular risks, but this was downplayed.
- The Data: It is estimated that Vioxx caused between 88,000 and 140,000 excess cases of serious heart disease in the USA alone before it was withdrawn in 2004. (Source: The Lancet, Graham et al., 2005 , Lancet Editorial).
The Difference: In Science, when we fail (like Vioxx), the data eventually comes out, the drug is pulled, and the system corrects itself. In pseudoscience, the failure is usually blamed on the patient (“You didn’t chant correctly”).
4. Unethical Trials: Similar to all other human efforts, when the power of scientific experiments falls into wrong hands, it may result in a disastrous and disturbing outcome. One such was Tuskegee Syphilis Study (1932-1972). This was a chapter of profound darkness.
The study intended to observe the natural progression of untreated syphilis in African American men, with a specific focus on comparing outcomes to white populations, based on racist beliefs that the disease affected the two races differently. In Macon County, Alabama, the U.S. Public Health Service enlisted 600 African American men, sharecroppers, tied to the land, under the guise of receiving free healthcare. Of these, 399 suffered from syphilis, while 201 served as a control group. They were told they were being treated for “bad blood,” a local colloquialism. In truth, they were being observed like specimens in a jar, denied the very cures that could save them.
The most harrowing aspect of this forty-year observation was not merely the deception, but the withholding of salvation. By the late 1940s, penicillin had become the standard cure. Yet, researchers actively blocked these men from receiving it, even intervening to prevent treatment when 256 of them were drafted during World War II. The human cost was devastating. By the time the study was exposed by whistleblower Peter Buxtun in 1972, 28 men had died directly from the disease, and another 100 from related complications. The tragedy rippled outward, infecting 40 wives and resulting in 19 children born with congenital syphilis.
The outcry led to a $10 million settlement and revolutionized research ethics, birthing the Institutional Review Boards we rely on today. But the scars remain, etching a deep distrust between the African American community and the medical establishment.
Besides this many western countries have unceasingly nurtured a racist idea of trying drugs and vaccines on humans from underdeveloped countries. This is an ongoing debate about colonialist attitudes in global health, where African children are sometimes used for research that would not be approved in the United States. This in terms created vaccine hesitancy. As an example, in Nigeria, in 2003, polio vaccination campaigns were boycotted due to fears that the vaccine was contaminated with anti-fertility agents.
5. What’s Wrong with Ayurveda?
If EBM has flaws, Ayurveda has structural failure. The issue is not that herbs are bad, plants are chemical factories. The issue is the lack of rigor and safety. There is a saying in India, that if Ayurveda does not cure diseases, it will not harm. This is simply not true.
1. Heavy Metal Toxicity This is the most critical immediate danger. Traditional formulations, especially Rasa Shastra, deliberately add mercury, lead, and arsenic, claiming that “purification” (samskaras) renders them safe. Chemistry disagrees. Lead is lead.
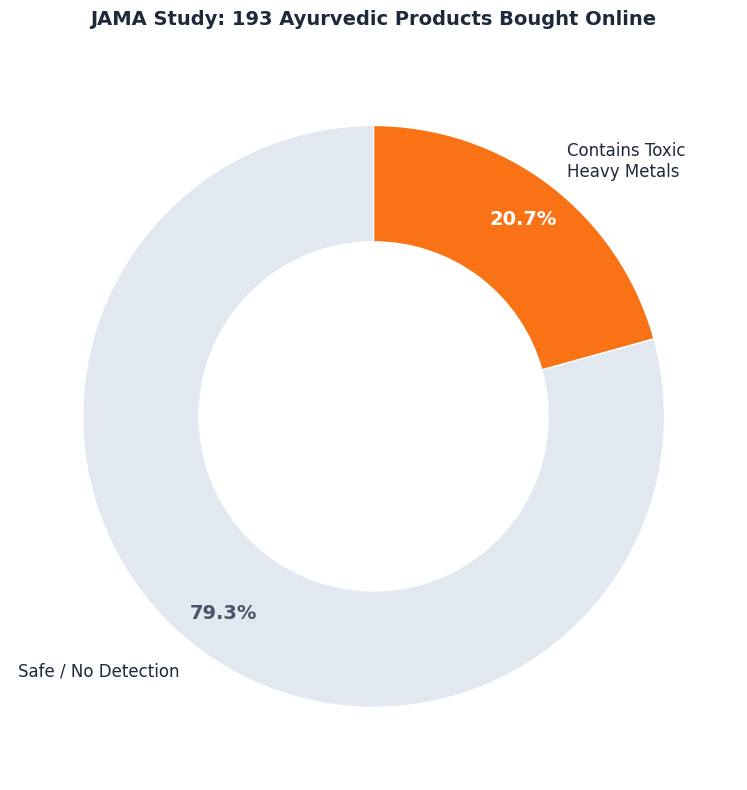
- The Source: A landmark study in the Journal of the American Medical Association (JAMA) (Saper et al., 2008) purchased 193 Ayurvedic products online. They found that 20.7% contained detectable lead, mercury, or arsenic. All strictly above safe limits.
- The Consequence: Lead poisoning causes permanent cognitive decline. We are seeing cases of “Ayurvedic Lead Encephalopathy”. This refers to severe brain damage (encephalopathy) resulting from lead poisoning caused by consuming certain Ayurvedic medicines.
2. No “Kill Switch” for Bad Ideas: Science is iterative. We used to perform lobotomies; we realized they were bad; we stopped. Ayurveda relies on the authority of the ancients. If the Charaka Samhita says it, it is Truth.
- The Problem: There is no mechanism in Ayurveda to say, “The sages were wrong about this.” This leads to the persistence of dangerous practices, like using heavy metals or treating serious infections with diet changes.
Falsifiability is the unique quality of any effective scientific paradigm.
3. Lack of Double-Blind RCTs: While there are studies on Ayurvedic herbs (like Ashwagandha), there is almost zero credible evidence for the system of Ayurveda. There are no randomized controlled trials proving that diagnosing someone as “Pitta-dominant” leads to better clinical outcomes than a placebo.
6. The Rational Wager: Why Governments Choose EBM
So, why should a government invest billions in hospitals, vaccines, and MRI machines (EBM) rather than expanding traditional healing centers?
It comes down to the Rational Wager.
Evidence Based Medicine, despite its corporate flaws, delivers consistent, measurable population-level results. Traditional medicine does not.
The Economic Reality: A sick population cannot build an economy.
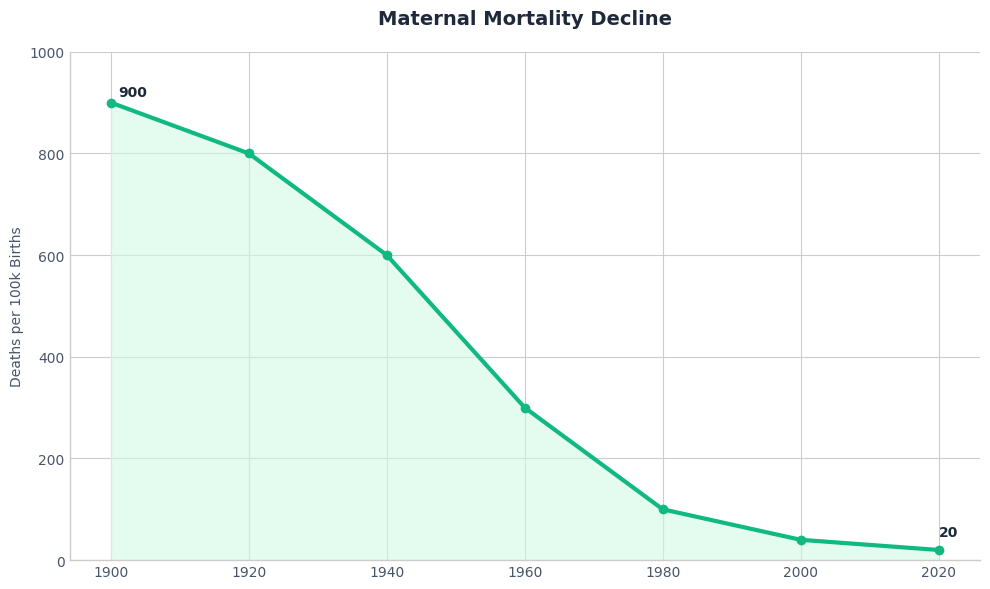
- Maternal Mortality: In 1900, for every 100,000 births, roughly 600-900 women died. Today, in developed nations using EBM, that number is roughly 10-20. That is EBM (sanitation, antibiotics, c-sections) at work.
- Antibiotics: Before penicillin, a scratch from a rose thorn could kill a prime minister. The introduction of antibiotics added nearly 10-15 years to the average human lifespan globally.
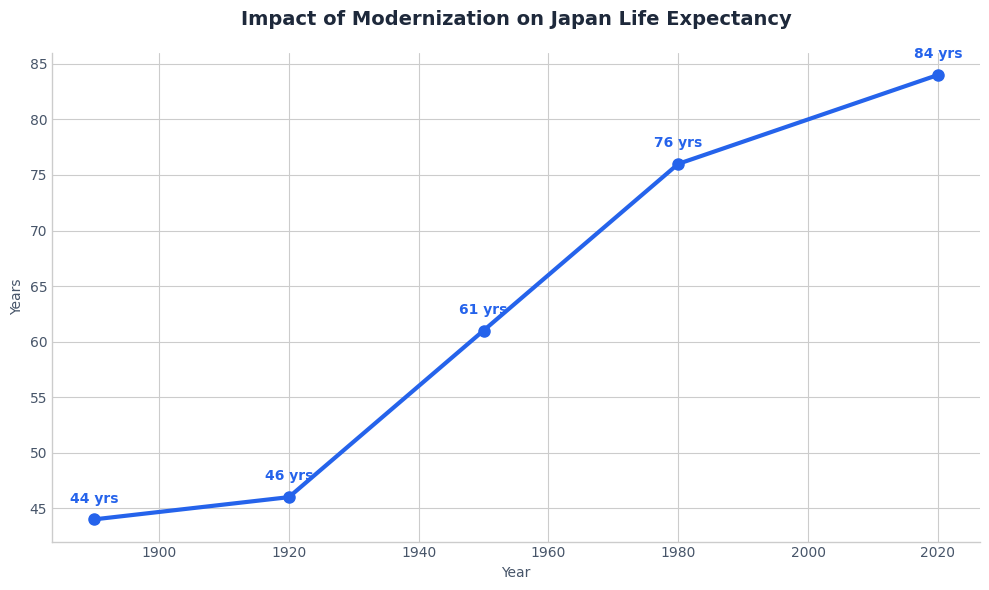
The Japanese Pivot (The Meiji Restoration): In the late 19th century, Japan looked at the world. They saw that Western armies were losing fewer soldiers to disease than Japanese armies.
- The Pivot: The Meiji government made a hard decision. They adopted German-style medical education and relegated Kampo (Japanese traditional medicine) to a secondary role.
- The Result: Japan now has one of the highest life expectancies in the world (84+ years).
The China Model (Pragmatism) China promotes Traditional Chinese Medicine culturally, but look at their actions. When SARS-CoV-2 hit Wuhan, they didn’t rely on acupuncture. They built massive negative-pressure hospitals, utilized ventilators, and raced for a vaccine based on mRNA or inactivated virus technology. They use EBM for critical care because EBM works when the stakes are highest.
Conclusion: Prioritize Evidence Based Medicine
We should not discard traditional medicine entirely. It is a rich source of hypotheses. We should mine it for molecules, as we did for Artemisinin. We should respect the emphasis on diet and lifestyle, which EBM often ignores.
But let us be clear: “Alternative Medicine” that has been proved to work is simply called “Medicine.”
Science is not a Western construct. It is a human one. It belongs to the Indian statistician as much as the British biologist. To choose Evidence-Based Medicine is not to betray one’s culture; it is to honor the greatest gift evolution gave us: the ability to question, to test, and to improve.
Keep an open mind, but not so open that your brains fall out.
Author’s Note: All statistical claims in this article are verifiable through the citations provided. Medical decisions should always be made in consultation with a qualified medical doctor (MD/MBBS).





